Jump to topic
Search
Program Details
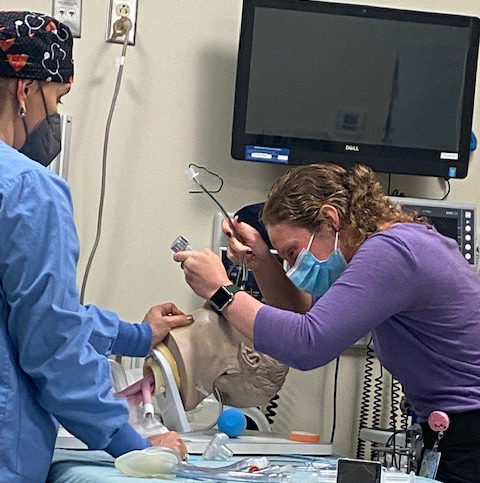
Jennifer King Wilson, MSN, AGACNP, CRNA, left, and APP fellow Katherine Pavlos PA-C, are pictured. Pavlos is performing an endotracheal intubation.
Penn State Health’s Advanced Practice Provider Critical Care Fellowship is a post–graduate, transition-to-practice training program for physician assistants and acute care nurse practitioners who have a sincere interest in a career as a critical care APP.
The 12-month program includes clinical rotations through Penn State Health’s adult critical-care units. In addition, trainees will have clinical experiences with services that are integral in supporting critical care including nephrology, palliative care and infectious disease. Trainees are expected to work a minimum of 36 hours per week clinically.
In addition to the variety of clinical experiences, there are didactic sessions as well as hands-on in the high-fidelity Clinical Simulation Center. Learning will also be enhanced using online learning modules, case conferences, evidenced-based readings and journal clubs. The trainee can expect to dedicate approximately 10 to 12 hours a week completing these learning activities.
Learn More about the Fellowship
General Applicant Information
The program is affiliated with Penn State Health Milton S. Hershey Medical Center, and fellows are hired as full-time employees with benefits, which includes a Continuing Medical Education allowance. Applicants must be graduates of an accredited nurse practitioner or physician assistant program, and board-certified through one of the major accrediting bodies specific to their discipline.
To apply for the APP Critical Care Fellowship, applicants must provide the following items:
- A personal statement, to include the applicant’s purpose in fellowship study and future professional goals as they relate to Critical Care.
- An updated curriculum vitae, to include a detailed description of prior critical care experience, if applicable.
- Minimum of three letters of recommendation, at least one from current or recent supervising physician or advanced practice clinician (nurse practitioner or physician assistant).
- An application through the Human Resources website.
Virtual Tour
Penn State Health
Penn State Health is a multi-hospital health system serving patients and communities across 29 counties of Pennsylvania. Its mission is to improve health through patient care, research, education and community outreach.
In December 2017, the system partnered with Highmark Health to facilitate creation of a value-based, community care network in the region. The shared goal of Highmark and Penn State Health is to ensure patients in the community are within:
- 10 minutes of a Penn State Health primary care provider
- 20 minutes of Penn State Health specialty care
- 30 minutes of a Penn State Health acute care facility
Learn more about Penn State Health

Penn State Health Children’s Hospital (left), Penn State Health Milton S. Hershey Medical Center (center) and Penn State Cancer Institute (right)
Penn State Health Milton S. Hershey Medical Center
500 University Dr., Hershey, Pa., 17033 (Derry Township, Dauphin County)
- The health system’s 647-bed flagship teaching and research hospital
- The only medical facility in Pennsylvania accredited as both an adult and a pediatric Level I (highest-level) trauma center
- Dedicated surgical, neuroscience, cardiovascular, trauma and medical intensive care units
- Accredited Life Lion critical-care transport providing more than 1,100 helicopter and approximately 750 ground ambulance transports per year
- More than 1,300 faculty members and more than 650 residents and fellows
- Approximately 29,000 admissions, 73,000 emergency department visits, 1.1 million outpatient visits and 33,000 surgical procedures annually
- Designated as a Magnet hospital since 2007
Learn more about Milton S. Hershey Medical Center
Penn State Health Children’s Hospital
600 University Dr., Hershey, Pa. 17033 (Derry Township, Dauphin County)
- An eight-story, 263,000-square-foot-facility built in 2013 and expanded in 2020
- 146 licensed pediatric beds, 18 acute care beds and a 56-bed neonatal intensive care unit
- Level IV (highest-level) neonatal intensive care unit
- Level I quaternary (highest-level) pediatric intensive care unit
- Level I (highest-level) pediatric trauma center designation
- Intermediate care unit
- Dedicated pediatric operating rooms
- More than 150,000 pediatric outpatient visits and approximately 5,000 pediatric patient discharges annually
Welcome to Hershey
More About Hershey
Interested in learning more about living and working in Hershey, Pa.? See details here:
Fellow wellness, including emotional, spiritual, social and physical health, is a crucial component to training and to becoming a professional, compassionate and resilient physician. Self-care is a skill which must be continually practiced and reinforced. Penn State College of Medicine and Penn State Health are committed to addressing wellness, with multiple resources readily available.
Institutional resources
Institutional Resources
Penn State Health and Penn State College of Medicine celebrate, embrace and support the diversity of all patients, faculty, staff, students and trainees.
Office for Diversity, Equity and Inclusion
In keeping with this, Penn State Health has an active Office for Diversity, Equity and Inclusion with various programs, networks and resource groups, including:
- Talks and lectures on diversity, equity and inclusion through the Inclusion Academy
- Regular events on topics such as eradicating racism and creating a culture of inclusiveness
- Many Business Employee Resource Groups (BERGs), including:
- Disability Business Employee Resource Group
- Interfaith Business Employee Resource Group
- LGBTQ+ Business Employee Resource Group
- Military and Veterans Business Employee Resource Group
- Multicultural Business Employee Resource Group
- NextGen Business Employee Resource Group
Learn more about the Penn State Health Office for Diversity, Equity and Inclusion
Learn more about the College of Medicine’s Office for Diversity, Equity and Belonging
Office for Culturally Responsive Health Care Education
The vision at Penn State College of Medicine and Penn State Health is to equip learners with the knowledge, skills and attitudes they will need to provide culturally excellent health care and research for an increasingly diverse U.S. population. The Office for Culturally Responsive Health Care Education was formed to help meet that goal.
Learn more about the Office for Culturally Responsive Health Care Education
Office for a Respectful Learning Environment
In addition, the institution does not tolerate discrimination, biases, microaggression, harassment or learner mistreatment of any kind, and any concerns are immediately addressed by the Office for a Respectful Learning Environment.
Learn more about the Office for a Respectful Learning Environment
Network of Under-represented Residents and Fellows
The Network of Under-represented Residents and Fellows (NURF) is a group of diverse residents and fellows representing all specialties. NURF’s goal is to promote cultural diversity in the residency programs through community involvement, mentorship with diverse faculty, professional networking and support for the recruitment of diverse medical students into the residency programs.
NURF is sponsored by the Penn State College of Medicine Graduate Medical Education Office and the Penn State Health Office for Diversity, Equity and Inclusion.
Curriculum Details
The fellowship’s mission is to provide a structured, comprehensive, transition-to-practice program to enhance the knowledge and skills of APPs who will serve the health needs of critically ill adults.
- Expand the knowledge and skills of novice APPs in order to provide safe, high-quality, cost-effective and evidence-based care to critically ill adults.
- Cultivate the APP leaders of the future, who will inspire innovation and share knowledge that will benefit all.
- Increase the confidence of APP trainees in performing procedures and therapeutic interventions.
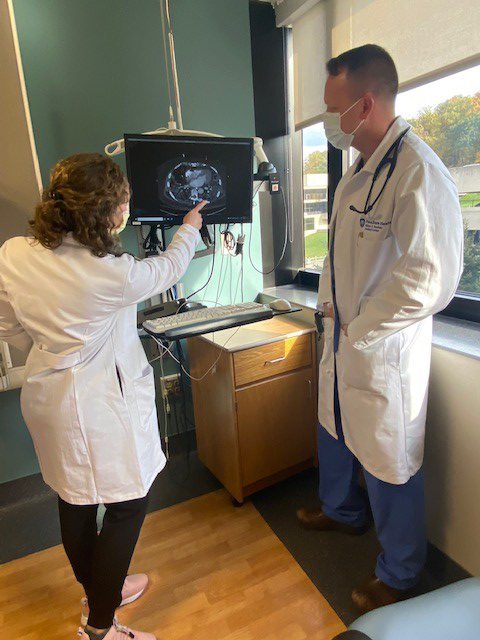
Katherine Pavlos, PA-C, and Ed Stene, AGACNP-BC, both APP Critical Care fellows, review a CT scan of the chest.
- Anesthesia surgical critical care
- Neuroscience intensive care
- Heart and vascular intensive care
- Medical intensive care
- Nephrology
- Infectious disease
- Palliative care
- Interventional pulmonary
- Medical emergency team
- Elective (six weeks)
- Trauma services
Note: These clinical rotations are subject to change.
- Advanced trauma life support
- Emergency neurological life support
- Fundamental critical care support
- Bedside ultrasound
- Clinical simulation (skills lab and OSCEs)
- Professional development and mentoring
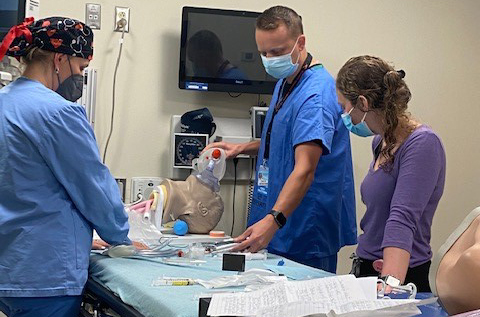
Ed Stene, AGACNP, and Katherine Pavlos, PA-C, APP Critical Care fellows, practice airway skills in the simulation center under the direction of Jennifer King Wilson, AGACNP, CRNA.
Procedures to be performed include, but are not limited to:
- Central line insertion
- Arterial line insertion
- Pulmonary artery catheter insertion
- Endotracheal intubation
- Bedside ultrasound for hemodynamic assessment
- Chest tube insertion
- Thoracentesis
- Satisfactory review on all end of rotation clinical evaluations.
- Obtain minimum grade of 85 percent on end-of-rotation quizzes.
- Completion of one scholarly project (e.g., manuscript submission to a professional journal or completion of QI or research project with abstract submission to a state or national meeting of a professional organization).
- Satisfactory completion of all OSCEs (clinical simulations).
- Attendance at two advanced practice council meetings.
- Attendance at one advanced practice grand rounds.
- Presentation of monthly case conference assigned.
- Facilitation of journal clubs as assigned.
- Completion of FCCS course (as available).
- Completion of ATLS course (as available).
- Completion of ENLS course (as available).
Evaluations will be completed by the clinical mentors at the end of each clinical rotation. End-of-rotation quizzes will also be administered. In addition, quarterly evaluations will be completed by the program director to ensure satisfactory progression in the program, as well as discuss trainee professional goals.





