Jump to topic
Search
Program Details
The Neonatal-Perinatal Medicine Fellowship at Penn State Health Children’s Hospital provides physicians with unrivaled training in neonatology with a comprehensive, innovative educational curriculum, as well as an in-depth research experience individually tailored to each trainee’s area of interest.
The fellowship, ACGME-accredited since 1984, has a proud history of graduating successful neonatologists in both academic and private-practice settings. The academic curriculum provides training in clinical and basic science research methodology, quality improvement, educational methodology and multidisciplinary team leadership. Fellows receive protected learning time for didactic lectures, simulation and research.
As the only Level IV neonatal intensive care unit (NICU) and referral center in central Pennsylvania, Penn State Health Children’s Hospital has a full complement of pediatric medical and surgical subspecialists. Specific therapies offered in the NICU include, but are not limited to:
- High-frequency ventilation
- Invasive and non-invasive neurally adjusted ventilatory assist (NAVA)
- Total-body cooling for hypoxic ischemic encephalopathy
- Extracorporeal membrane oxygenation (ECMO)
With nearly 800 admissions annually, including an active transport team and an obstetrical service with more than 2,200 deliveries per year, the patient population has a strong combination of patient acuity, diversity and complexity. The Complex Fetal Care Center attracts a diverse mix of complicated pregnancies, and the new, state-of-the-art 56-bed NICU opened in November 2020.
The medium-sized academic program offers fellows a combination of a personalized fellowship experience with all that an academic medical center has to offer. The group includes approximately 30 neonatologists and advanced practice providers and a sizable clinical and support staff. Program faculty are nationally and internationally recognized in many areas of clinical, basic, translational and quality improvement research in many areas, including autonomic regulation, neonatal hypoglycemia, neonatal neurology, neonatal abstinence syndrome and pulmonary immunology.
Fellows in the training program develop a strong foundation of medical knowledge in neonatal physiology and pathophysiology and learn to provide evidence-based treatment strategies within a family-centered care model. Faculty and co-fellows support each fellow through their training with one-on-one mentoring and supervision, allowing for increased independence as skills progress. At the end of three years, the program’s goal is for fellows to have the knowledge and skills to provide top-notch and compassionate neonatal care.
Learn More about the Fellowship
Dear aspiring fellow,
Welcome! I invite you to explore this website to find out more about the Neonatal-Perinatal Medicine Fellowship at Penn State Health Children’s Hospital. Please be sure to follow the links to our Neonatal Intensive Care Unit (NICU), faculty and fellow pages, and the Hershey area.
Why choose Penn State? As a medium-sized program with access to a nationally-recognized quaternary care medical center and medical school, our fellows obtain experience managing a wide range of neonatal pathologies while receiving individual attention from faculty. Our size also allows us to tailor fellow training based on their interests, skills and career goals. Our Neonatal-Perinatal Medicine Fellowship has a proud history of training successful academic and clinical neonatologists since 1984.
Our recruitment and interview process continues to be virtual, but we are excited to show you all that our program has to offer!
Please don’t hesitate to contact me with any questions. I look forward to meeting you.
Kristen M. Glass, MD
Associate Professor of Pediatrics
Program Director, Neonatal-Perinatal Medicine Fellowship
kglass1@pennstatehealth.psu.edu
717-531-8413
Update for the 2024 Interview Season
In accordance with national recommendations and in fairness to all fellowship candidates, all interviews will be held virtually.
General Application Information
The Neonatal-Perinatal Medicine Fellowship participates in the National Residency Matching Program (NRMP) Pediatric Subspecialties Match, with typically two fellowship spots per year.
All application materials must be submitted through the Electronic Residency Application Service (ERAS) for fellowship applicants. Applicants are encouraged to complete their applications as soon as possible once ERAS opens for the season.
All applicants must have completed a residency from an ACGME-certified training program.
Eligibility
Qualified candidates will be:
- U.S. citizens, permanent residents or J-1 visa holders (no additional visa types are sponsored)
- Board-eligible or board-certified in pediatrics
- Eligible for a Pennsylvania medical training license
Required Supporting Documents
The following documents should be uploaded to ERAS for review:
- ERAS application, including current photograph
- Personal statement
- Curriculum vitae
- USMLE or COMLEX transcript
- ECFMG certificate (if applicable)
- Three letters of recommendation, including one from a neonatologist and one from the applicant’s current residency program director
International students
International medical graduates must hold a currently valid certificate from the Educational Commission for Foreign Medical Graduates (ECFMG) to be considered for the match. The program accepts J-1 visas only.
A directory of clinical faculty is seen here. See research faculty and publications from Maternal-Fetal Medicine here.
About the fellow

Brandon Costello, DO
Name: Brandon Costello, DO
Hometown: Hamburg, NY
Clinical interests: Transport Medicine and ECMO
Research interests: As a General Pediatrician who’s spent the past several years in a resource-limited area, I’m interested in ways to improve community hospital-level capabilities to support unexpected premature deliveries or newborn complications to optimize outcomes prior to transfer to a higher level of care.
Why did you choose Neonatology?
I always pictured myself as a “small-town” doc who got to know his patients and their families on a personal level, but I struggled with the fact that I also loved ICU medicine and the complex pathophysiology associated with it. Neonatology ironically combines the best of both worlds. The transitional physiology from fetus to newborn and ongoing development found in the NICU is unlike any other type of medicine, and the prolonged hospitalizations associated with this type of medicine allow you to get to know your patient and build a foundation of trust with their families, like a general practitioner, during this stressful time.
Why did you choose Penn State for your fellowship training?
As a Penn State undergraduate alumni, I was eager to come back to this community. Penn State offers some unique opportunities not available in other training programs including an active transport medicine program with robust fellow involvement, a diverse patient population with an increased prevalence of rarer genetic disorders, and ECMO in the unit with active management by the neonatology team. The fact that the unit is not fellow-dependent also means that more focus can be placed on learning and honing skills rather than just completing the day-to-day tasks. As someone who’s recently become a dad, I appreciate the support the staff and fellows have offered during my transition and feel that the program is very family oriented.
What am I most excited about starting fellowship
After practicing as a General Pediatrician for the past 4 years, I’m excited to be able to focus on the subpopulation of patients that I truly have a passion for.
What do you enjoy doing outside of work? How is life in Hershey, Pa.?
My wife and I recently welcomed our first child into the world, so currently naps and diaper changes are high on the priority list, but I love to cook/bake when I get the chance as well as explore the outdoors. I am a huge fan of water sports and hiking. I grew up just down the road from a dairy farm, so Hershey PA feels like home. It’s a small rural town with a very welcoming and quiet feel. It’s a great place to start/raise a family, and if you are looking for some bigger city living, Harrisburg and Philadelphia are easy driving distances away.
About the fellow

Danielle Smith, MD
Name: Danielle Smith, MD
Hometown: Toledo, Ohio
Clinical interests: Neonatal abstinence syndrome, congenital cardiac defects, medical student and resident education, family communication
Research interests: NAS/NOWS, neonatal pain management
Why did you choose Neonatology?
“I enjoy the mixture of high and low acuity that neonatology offers; it makes each day different. It is incredibly rewarding to care for a patient from start to finish, and watch them progress and improve.”
Why did you choose Penn State for your fellowship training?
The short answer is that I like it here – the providers, nurses, and respiratory therapists make this a great place to work and learn. I completed my residency training at Penn State, and so knew firsthand how wonderful the team is. This institution offered me the opportunities I was looking for to grow in my professional and personal life. I knew I would be challenged in important areas and supported to pursue my interests.”
What are your thoughts on fellowship so far?
“It has been a whirlwind jumping back in from maternity leave! The senior fellows and mentorship program have been a huge support in getting me settled and set up for success.”
What do you enjoy doing outside of work? How is life in Hershey, Pa.?
“Snuggling with my baby! I also dabble in sourdough and baking cookies. My husband and I enjoy all of the hiking and walking trails around here. It is a scenic, beautiful place to live.”
Testimonials from Graduates of Penn State Neonatal-Perinatal Medicine Fellowship Program
Lynnlee Depicolzuane, DO
Sinai Hospital of Baltimore, Baltimore, MD
Penn State NPM Fellow 2019-2022
Penn State has always been special to me, having completed undergraduate training at main campus. When I matched there for fellowship, I could not have been happier, knowing the commitment to education of the institution. I was well prepared for my transition to attending life after my training, having experienced continued advancement in autonomy along with full support from the attendings and advanced practitioners. I was able to see a wide variety of cases with a truly multi-disciplinary team and participate in critical care transports, preparing me for any clinical position in the future. My research experience was also valuable, with strong support from the division for attendance at academic meetings and two resulting publications. I would recommend training at Penn State Hershey for anyone looking for a well-rounded program.
Tracey Harris, DO
Einstein Hospital, Philadelphia, PA
Penn State NPM Fellow 2016-2019
As my June 2019 graduation approached, I was frequently asked if I was nervous to embark upon my new role as an attending neonatologist. The simple answer was no, because I was extremely well-prepared by my fellowship training at Penn State. Not only is there an abundance of pathology in the NICU at Penn State, ranging from extreme prematurity to complex congenital conditions, but the faculty and staff are extremely invested in education. After practicing in a busy Level 3 NICU since leaving Hershey, I am even more thankful for my fellowship experience and would highly recommend the program at Penn State to anyone beginning their training in Neonatology.
Payal Trivedi, DO
Temple University Hospital/St. Christopher’s Hospital for Children, Philadelphia, PA
Penn State NPM Fellow 2015-2018
I have had the opportunity to work in both private practice and academic settings. The training I received at Penn State helped me to develop adaptability, which was critical in transitioning between these two work environments. As a fellow, I gained confidence leading a team in the delivery room and while on transports of critically ill infants. I am particularly grateful for the experience as an acting attending during my third year fellowship, which made the transition to being a new attending much less daunting. I have received positive feedback on multiple occasions from colleagues, mid-level staff, and nurses about my approach to providing updates or having difficult conversations with families. I would choose Penn State again over other programs because the fellowship training provided me with a very broad experience in neonatology, from extremely low birth weight infants to full term babies with rare anomalies. Everyone has a stake in education, from the faculty to the respiratory therapists and clinical pharmacists, making multidisciplinary family-centered rounds insightful and educational. During my training at Penn State I developed long-lasting relationships with people whom I can reach out to for advice even after fellowship.
Richard Jack, MD
Kapiolani Medical Center for Women & Children, Honolulu, HI
Penn State NPM Fellow 2014-2017
The Neonatal-Perinatal Medicine Fellowship at Penn State Milton S. Hershey Medical Center is a strong program with an excellent environment for learning. The attendings, NNPs and PAs are all a pleasure to work with. There is a nice balance of clinical and research exposure. As a referral center, the NICU sees a vast range of pathology and acuity which is excellent for training. The fellows are well respected and given appropriate autonomy for patient care. The nurses and respiratory therapists are knowledgeable and I learned a lot from them as well. I especially enjoyed my experiences with neonatal transport and ECMO. I would strongly recommend this program as I feel that it has prepared me well for attending life.
Jeffrey Meyers, MD
Golisano Children’s Hospital, University of Rochester, Rochester, NY
Penn State NPM Fellow 2009-2012
I loved my experience at Penn State. There is a diverse exposure to complex pathophysiology from a large catchment area in PA. I benefitted from exposure to ECMO, complex congenital heart disease, and rare genetic disorders. The faculty provided excellent bedside teaching, and supported the development of independence and autonomy among the fellows. There was also a structured approach to supporting fellowship scholarly activities. Hershey, PA is a beautiful place to live and raise a family! I wouldn’t change a thing about my experience or where I trained.

Virtual Tour
Penn State Health
Penn State Health is a multi-hospital health system serving patients and communities across 29 counties of Pennsylvania. Its mission is to improve health through patient care, research, education and community outreach.
In December 2017, the system partnered with Highmark Health to facilitate creation of a value-based, community care network in the region. The shared goal of Highmark and Penn State Health is to ensure patients in the community are within:
- 10 minutes of a Penn State Health primary care provider
- 20 minutes of Penn State Health specialty care
- 30 minutes of a Penn State Health acute care facility
Learn more about Penn State Health

Penn State Health Children’s Hospital (left), Penn State Health Milton S. Hershey Medical Center (center) and Penn State Cancer Institute (right)
Penn State Health Milton S. Hershey Medical Center
500 University Dr., Hershey, Pa., 17033 (Derry Township, Dauphin County)
- The health system’s 628-bed flagship teaching and research hospital
- The only medical facility in Pennsylvania accredited as both an adult and a pediatric Level I (highest-level) trauma center
- Dedicated surgical, neuroscience, cardiovascular, trauma and medical intensive care units
- Accredited Life Lion critical-care transport providing more than 1,100 helicopter and approximately 750 ground ambulance transports per year
- More than 1,300 faculty members and more than 650 residents and fellows
- Approximately 28,500 admissions, 75,000 emergency department visits, 1.1 million outpatient visits and 32,000 surgical procedures annually
- Designated as a Magnet hospital four consecutive times, one of 116 hospitals to do so
Learn more about Milton S. Hershey Medical Center
Penn State Health Children’s Hospital
600 University Dr., Hershey, Pa. 17033 (Derry Township, Dauphin County)
- A five-story, 263,000-square-foot-facility built in 2013
- Three-floor expansion opened in November 2020
- 146 licensed pediatric beds, 18 acute care beds and a 56-bed neonatal intensive care unit
- Level IV (highest-level) neonatal intensive care unit
- Level I (highest-level) pediatric trauma center designation
- Dedicated pediatric operating rooms
- More than 150,000 pediatric outpatient visits and approximately 5,000 pediatric patient discharges annually
Welcome to Hershey
More About Hershey
Interested in learning more about living and working in Hershey, Pa.? See details here:
Wellness, including emotional, spiritual, social and physical health, is a crucial component to training and to becoming a professional, compassionate and resilient physician. Self-care is a skill which must be continually practiced and reinforced. Penn State College of Medicine and Penn State Health are committed to addressing wellness among residents and fellows, with multiple resources readily available.
Institutional resources
- Visit BeWell – a health program designed to support Penn State Health employees
- See Penn State College of Medicine wellness resources here
- Employee Health Care Concierge and Case Management Service
- Partners in Medicine
Moving to a new city with your family does not have to be stressful. Residency programs have assisted many significant others with finding employment. There is also a GME-Wide Partners in Medicine (PIM) group that offers networking opportunities as well as various social and community oriented activities. - The Doctors Kienle Center for Humanistic Medicine
- Active and easily accessed Office of Professional Mental Health
Graduate medical education resources
Department and Division Resources
The division recognizes the importance of maintaining a healthy work-life balance. Throughout the year, the division hosts celebrational gatherings, including an annual new fellow welcome picnic as well as a holiday party and fellow graduation picnic.

Wellness activity

Wellness activity

Graduation celebration

Holiday celebration
Institutional Resources
Penn State Health and Penn State College of Medicine celebrate, embrace and support the diversity of all patients, faculty, staff, students and trainees.
Office for Diversity, Equity and Inclusion
In keeping with this, Penn State Health has an active Office for Diversity, Equity and Inclusion with various programs, networks and resource groups, including:
- Talks and lectures on diversity, equity and inclusion through the Inclusion Academy
- Regular events on topics such as eradicating racism and creating a culture of inclusiveness
- Many Business Employee Resource Groups (BERGs), including:
- Disability Business Employee Resource Group
- Interfaith Business Employee Resource Group
- LGBTQ+ Business Employee Resource Group
- Military and Veterans Business Employee Resource Group
- Multicultural Business Employee Resource Group
- NextGen Business Employee Resource Group
Learn more about the Penn State Health Office for Diversity, Equity and Inclusion
Learn more about the College of Medicine’s Office for Diversity, Equity and Belonging
Office for Culturally Responsive Health Care Education
The vision at Penn State College of Medicine and Penn State Health is to equip learners with the knowledge, skills and attitudes they will need to provide culturally excellent health care and research for an increasingly diverse U.S. population. The Office for Culturally Responsive Health Care Education was formed to help meet that goal.
Learn more about the Office for Culturally Responsive Health Care Education
Office for a Respectful Learning Environment
In addition, the institution does not tolerate discrimination, biases, microaggression, harassment or learner mistreatment of any kind, and any concerns are immediately addressed by the Office for a Respectful Learning Environment.
Learn more about the Office for a Respectful Learning Environment
Network of Under-represented Residents and Fellows
The Network of Under-represented Residents and Fellows (NURF) is a group of diverse residents and fellows representing all specialties. NURF’s goal is to promote cultural diversity in the residency programs through community involvement, mentorship with diverse faculty, professional networking and support for the recruitment of diverse medical students into the residency programs.
NURF is sponsored by the Penn State College of Medicine Graduate Medical Education Office and the Penn State Health Office for Diversity, Equity and Inclusion.
Mailing Address
Penn State Health Children’s Hospital
Neonatal-Perinatal Medicine Fellowship
500 University Dr.
P.O. Box 850
Mailcode H085
Hershey, Pa. 17033
General Contact Information
Phone: 717-531-5458
Curriculum Details
The Neonatal-Perinatal Medicine Fellowship is a three-year, ACGME-accredited training program. Fourteen months are dedicated to subspecialty clinical training, designed for the trainee to develop the necessary knowledge and skills for the practice of neonatology. These months include two required rotations in pediatric cardiology and maternal-fetal medicine. The curriculum is structured to give fellows more responsibility and independence as they gain experience and skill. During their third year, fellows on clinical service are placed in the role of acting attending with appropriate supervision from attending physicians.
Also, 19 months of the fellowship program are dedicated to clinical or basic science research training. The goal of research training is to provide fellows with a skill set to support career-long investigation and scholarly contribution to the field of neonatal-perinatal medicine.
Fellows in the program are trained in providing prenatal consultation during clinical rotations under faculty supervision. They also see patients in neurodevelopmental clinic throughout all three years of their training, where they learn to evaluate for developmental delays in the most at-risk patients.
Neonatal-Perinatal Medicine fellows supervise and teach medical students, residents and learners from allied health professions on clinical rotations. Throughout all three years of training, fellows are expected to prepare and present formal lecture topics and clinical cases at divisional conferences.
The rotation schedule for each of the three years of fellowship is listed here. Schedules are customizable based on trainee interests, skills and goals. Fellows receive one month (four weeks) of vacation per year.
Year 1
- Orientation to service in the NICU – one month
- Service in the NICU – five months
- Neurodevelopmental follow-up clinic sessions – six half-days
- Research – five months
- Vacation – one month (four weeks)
- In-house calls – approximately 55
Year 2
- Service in the NICU – four months
- Maternal-fetal medicine – one month
- Neurodevelopmental follow-up clinic sessions – six half-days
- Research – six months
- Vacation – one month (four weeks)
- In-house calls – approximately 55
Year 3
- NICU as acting attending (with supervision) – three months
- Cardiology – one month
- Neurodevelopmental follow-up clinic sessions – six half-days
- Research – seven months
- Vacation – one month (four weeks)
- In-house calls – approximately 55
Summary over all three years of fellowship
- NICU service – 12 months
- Maternal-fetal medicine – one month
- Cardiology – one month
- High-risk neurodevelopmental follow-up clinic sessions – 18 half-days
- Research – 19 months
- Vacation – three months (12 weeks)
- In-house night calls (approximately one night in six, averaged over three years) – approximately 160
Typical day in the life of an on-service fellow
- 7 a.m. – Sign-out
- 7:30 to 9 a.m. – Patient care
- 9 a.m. – Team huddle, followed by family-centered multidisciplinary rounds
- Noon – Conference
- 1:15 p.m. – Radiology rounds with pediatric radiologist
- 2 to 4 p.m. – Patient care, family meetings and resident education
- 4 p.m. – Sign-out
The program’s size allows for flexibility for fellows to customize their training with additional experiences in the second and third years, including, but not limited to, an elective in palliative care medicine and medical education courses. Through partnership with Penn State College of Medicine, the program offers graduate certificates and advanced degree programs.
Cardiology and maternal-fetal medicine (MFM) are two required rotations in the educational curriculum.
MFM is a one-month rotation completed in the second year of fellowship. During this rotation, fellows spend two weeks on the MFM inpatient service and outpatient clinic, where they are exposed to fetal testing and monitoring modalities. For the remainder of the month, fellows participate in outpatient prenatal consultations referred by the Perinatal Center and the obstetric service.
The cardiology rotation is a one-month experience during the third year of fellowship on the inpatient cardiology and cardiothoracic surgery service in the cardiac intensive care unit. During this rotation, fellows also follow patients with congenital heart disease in the NICU, observe cardiac surgeries and see patients in fetal cardiology clinic.

Boot Camp participants
Incoming first-year fellows in our program participate in the Regional First-Year Fellow Boot Camp at Yale-New Haven Children’s Hospital. Penn State has participated in this regional bootcamp since 2010.
The course provides two days of didactics, simulation training, and networking with other new first-year fellows in neonatal-perinatal medicine from all over the Mid-Atlantic region. Registration, travel and meal costs are covered by the program and the sponsoring institution.
Weekly or Every Other Week
Pediatric Grand Rounds (Tuesdays)
Starting Tuesday mornings, Pediatric Grand Rounds covers core topics in pediatrics and pediatric subspecialties. Speakers include local and nationally-recognized faculty and researchers. Pediatric fellows also have the opportunity to speak at Grand Rounds during their third year of fellowship.
Journal Club (Wednesdays)
Twice monthly, the division meets to discuss recent literature in order to inform best practice. Fellow and faculty discussants lead the critical appraisal of one to two recent articles per session.
Fellows’ Physiology Lecture Series (Wednesdays)
Every other Wednesday, fellows and faculty facilitators meet to discuss physiology topics relevant to the Neonatal-Perinatal Medicine Board Examination. Each session concludes with a review of board-style questions. The curriculum is currently undergoing a transition from a traditional didactic model to a flipped-classroom model using content from the Organization of Neonatal-Training Program Directors (ONTPD) NeoFlip curriculum. Faculty from other specialties, including surgery, cardiology, pulmonology and maternal-fetal medicine, also present on relevant topics.
Morbidity and Mortality (Wednesdays)
Morbidity and Mortality is a multidisciplinary team discussion aimed at improving patient care, held every other Wednesday. Fellows are responsible for preparation and presentation of the case(s), including literature review, and discussion of systems improvements.
Perinatal Conference (Fridays)
Perinatal Conference is the multidisciplinary meeting between maternal-fetal medicine and neonatal-perinatal medicine groups to discuss recent and upcoming deliveries. Faculty and fellows from both specialties discuss cases as well as physiology and management of high-risk pregnancies. Topics relevant to both sides of the mother-fetus dyad are discussed with the goal of improving understanding and communication between members of this special care team.
Division Meeting (every other Thursdays)
On alternate Thursdays, the faculty, advanced practice providers and fellows gather to discuss relevant topics in neonatology in order to inform best practice in the NICU.
Monthly
Neonatal-Perinatal Medicine Scholarly Curriculum (second Wednesday)
The Scholarly Curriculum Series is held every second Wednesday of the month and is a fellow conference facilitated by a core group of faculty on topics including: biostatistics and epidemiology with hands-on experience using statistical software, research methodology, quality improvement, medical and research ethics and education methodology.

Trainees in the Neonatal-Perinatal Medicine Fellowship are seen with one of the Penn State Health Children’s Hospital visiting therapy dogs during a core curriculum event.
Fellows’ Core Curriculum Series (second Monday)
Fellows’ Core Curriculum is a set of structured didactic sessions held the second Monday of the month addressing aspects of the ACGME’s core curriculum required for all pediatric subspecialty training, as well as some life-after-fellowship topics. This innovative learning program brings together fellows from across the Department of Pediatrics and provides instruction on topics such as research methodology and study design, grantsmanship, manuscript writing, financial advisement, work-life balance and physician wellness, CV preparation and negotiating employment contracts.
Complex Fetal Care Center Meeting (first Tuesday)
The multidisciplinary Complex Fetal Care Center meeting is held on the first Tuesday of the month to discuss upcoming deliveries of patients in the Complex Fetal Care Center. These patients include mothers carrying fetuses with congenital heart disease and other congenital malformations, as well as twin-twin transfusion. Facilitated by the maternal-fetal medicine perinatal coordinators, the meeting includes a brief review of each maternal/fetal case currently cared for within the Perinatal Program, with in-depth multidisciplinary commentary and discussion as appropriate. Postnatal case correlation is also included.
Fellow Simulations (last Wednesday)
On the last Wednesday of the month, fellows participate in simulations focusing on the practice of clinical skills, as well as the development of communication and leadership skills. Scenarios range from management of congenital anomalies in the delivery room, to emergency situations in the NICU and delivery of difficult news to families.
Neonatal-Perinatal Medicine Research Conference (last Friday)
This conference is a divisional meeting typically held on the last Friday of the month at 2 p.m. to showcase both fellow and faculty research. The purpose of the conference is to provide updates on research projects going on within the division, to give feedback to the investigators to strengthen their projects as well as to provide inspiration and foster collaboration between researchers.
Fellows have opportunities throughout their training to participate in simulation-based education both in the NICU and in the nationally recognized and accredited Clinical Simulation Center.
Simulation is used regularly throughout the curriculum and is taught by faculty and staff trained in simulation education. Recurring simulations include procedural simulations such as exchange transfusion, thoracentesis and chest tube placement, quarterly ECMO simulations and monthly in-situ mock codes.
Fellows are encouraged to serve as facilitators for simulations held as part of medical student and pediatric resident education. These programs provide fellows with experience running simulation scenarios and facilitating educational debriefing sessions. Fellows are encouraged to obtain their certification as NRP instructors and to participate in NRP education for the NICU and obstetrical teams.
Additional training is available through the Teaching with Simulation instructor certificate course.
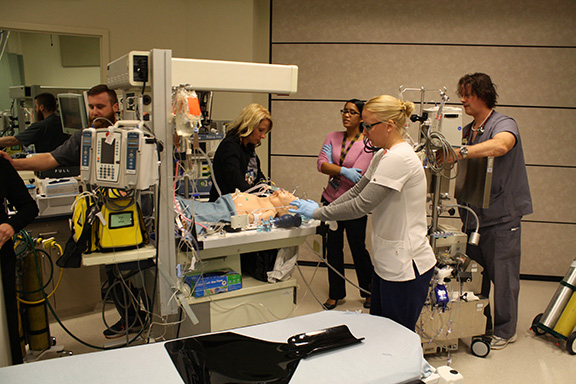
ECMO simulation
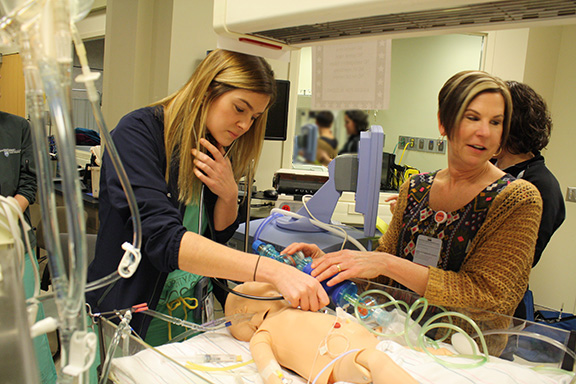
ECMO simulation
Mentoring is an essential part of professional development during fellowship and beyond. The training program starts fellows off on the right path with an onboarding mentorship program.
This program pairs incoming fellows with a faculty member who meets regularly throughout the first four months of fellowship to provide advice on adjusting to the fellow role, the medical center and life in Hershey. The onboarding mentor also helps fellows explore interests and goals and orients them to opportunities for involvement in committees, quality improvement teams and research.
At the end of the onboarding mentorship commitment (October of the first year of fellowship), fellows select an academic mentor from among the faculty. Academic mentors meet with fellows at least semi-annually to provide feedback on fellow evaluations and aid in the development of fellowship and career goals. Research mentors are also an important part of the fellow mentoring team. These mentors, selected based on fellow research interests and career goals, guide the fellow through a longitudinal research project along with the Scholarly Oversight Committee.
Meet the directors of our clinical research and basic science research programs:
 Dr. Doheny is the director of clinical research for the Division of Neonatal-Perinatal Medicine. Her research interests include clinical and translational approaches for integrating biomarkers and clinical data on stress regulatory systems. Her Newborn Biobehavioral Laboratory employs a staff of research technologists trained in techniques of biological and behavioral stress measures, including salivary hormone and buccal DNA sampling, heart rate variability (HRV), skin conductance, stress/pain behaviors, the modified Trier Social Stress Test, narrative interviews and health/psychological inventories. Dr. Doheny’s research is funded by an NIH R01 grant investigating vagal dysregulation in neonatal gastrointestinal pathology. She has successfully mentored many fellows in projects ranging from the role of zinc transporters breast milk nutrition to skin conductance and HRV in babies with neonatal abstinence syndrome.
Dr. Doheny is the director of clinical research for the Division of Neonatal-Perinatal Medicine. Her research interests include clinical and translational approaches for integrating biomarkers and clinical data on stress regulatory systems. Her Newborn Biobehavioral Laboratory employs a staff of research technologists trained in techniques of biological and behavioral stress measures, including salivary hormone and buccal DNA sampling, heart rate variability (HRV), skin conductance, stress/pain behaviors, the modified Trier Social Stress Test, narrative interviews and health/psychological inventories. Dr. Doheny’s research is funded by an NIH R01 grant investigating vagal dysregulation in neonatal gastrointestinal pathology. She has successfully mentored many fellows in projects ranging from the role of zinc transporters breast milk nutrition to skin conductance and HRV in babies with neonatal abstinence syndrome.
 Dr. Chroneos is the director of basic science research for the Division of Neonatal-Perinatal Medicine. His research focuses on understanding how surfactant proteins modulate host defense and inflammation in the lung, with a major current focus on influenza pathogenesis, host pathogen interactions and innate and adaptive immune responses to bacterial and viral infections. In addition to this work, Dr. Chroneos also studies the role of SP (surfactant protein)-A and SP-R210 in iron sequestration by alveolar macrophages and its impact in pulmonary host defense, the role of endophilin B2 in epithelial cell regeneration in response to lung injury and the mechanisms of alveolar simplification in response to hyperoxic injury. Dr. Chroneos has mentored and directed the research training of undergraduate and graduate students, medical students, postdoctoral and clinical fellows and junior faculty and has served on multiple doctoral committees for graduate students and mentoring committees for junior faculty.
Dr. Chroneos is the director of basic science research for the Division of Neonatal-Perinatal Medicine. His research focuses on understanding how surfactant proteins modulate host defense and inflammation in the lung, with a major current focus on influenza pathogenesis, host pathogen interactions and innate and adaptive immune responses to bacterial and viral infections. In addition to this work, Dr. Chroneos also studies the role of SP (surfactant protein)-A and SP-R210 in iron sequestration by alveolar macrophages and its impact in pulmonary host defense, the role of endophilin B2 in epithelial cell regeneration in response to lung injury and the mechanisms of alveolar simplification in response to hyperoxic injury. Dr. Chroneos has mentored and directed the research training of undergraduate and graduate students, medical students, postdoctoral and clinical fellows and junior faculty and has served on multiple doctoral committees for graduate students and mentoring committees for junior faculty.
Fellows are encouraged to write IRB applications and apply for internal and external grants as applicable to their research project. Fellows then participate in data collection and statistical analysis with the goal of developing at least one peer-reviewed manuscript for publication.
Fellows are also strongly encouraged to participate in Quality Improvement (QI) Projects as the lead of a multidisciplinary team. Many of these QI projects have led to publications and regional/national presentations.
The program highly encourages fellows to attend national, regional and local conferences to present their work and to interact with researchers and fellows from other institutions for inspiration, continuing education and initiating professional collaborations.
Below is a list of recent research and QI projects by our fellows:
Fellow Honors and Recognitions
Penn State College of Medicine and Penn State Health Milton S. Hershey Medical Center accept ongoing nominations for the Exceptional Moments in Teaching award.
The award, given monthly by the Office for a Respectful Learning Environment, accepts nominations from College of Medicine students who are invited to submit narratives about faculty members, residents, fellows, nurses or any other educators who challenge them and provide an exceptional learning experience. See more about the award here.
Previous nominees from the Neonatal/Perinatal Medicine Fellowship are listed here. Click the + next to a nominee name to read their nominator’s comments.
Pediatric Research Day is an every-other-year event that highlights the research of junior faculty and trainees at Penn State Health Children’s Hospital. Unfortunately, due to COVID 19, the conference was not held in 2021. This event is an opportunity for researchers and caregivers at Penn State College of Medicine, other Penn State campuses and in the community to discover new applications for their work or to talk about potential areas for collaboration.
Finalists for the Clinical Young Investigator Award are selected from abstracts submitted by medical students, residents, fellows and junior faculty.
Previous presentations from the Neonatal/Perinatal Medicine Fellowship are listed here, along with any honors or awards received.
The annual Resident/Fellow Research Day is held each year (with exception of during the COVID-19 pandemic) on and around the Penn State Health Milton S. Hershey Medical Center campus.
The intent of the event is to provide an opportunity for residents and fellows to showcase their research accomplishments to their peers in other clinical departments, as well as their colleagues in the basic sciences.
Learn more about Resident/Fellow Research Day here.
Previous presentations from the Neonatal/Perinatal Medicine Fellowship are listed here.
Latest News from Penn State Health Children's Hospital






